When I was a kid I often chose to walk about 50 minutes from my middle school to my house. There were two reasons for this. The first was the bus seemed to take this long anyway due to my stop being next to last on the route. In reality it probably took 30 vs 50 minutes, but this line of thinking helped support my real reason for walking:
There was this gas station called The Country Store that was a slight detour on my hike home. A quick stop meant I could get some tax free candy from the military Shopette. Usually, I filled a small paper sack with the stuff, which probably meant I came home with a good 2lbs (0.9 kg) of sweets.
Well, at least half of that would make it home… That half found its way into my dresser drawer to keep it away from my sisters and so I could snack on it over the next couple days. Once I ran out, it was back to the country store.
 I have always had a sweet tooth. If I think back, there were many signs that I should have taken it easy on the sugar. One was going from zero to eight cavities in one dentist visit! I promptly blamed this on a “greedy” dentist. He was an easy target as all the kids in his office looked like Jaws from the old James Bond movies. No exaggeration!
I have always had a sweet tooth. If I think back, there were many signs that I should have taken it easy on the sugar. One was going from zero to eight cavities in one dentist visit! I promptly blamed this on a “greedy” dentist. He was an easy target as all the kids in his office looked like Jaws from the old James Bond movies. No exaggeration!
The second sign was one day during summer break in college. I was heading to another students apartment, with a milk jug full of Kool-Aid (for myself). I took a swig and then immediately started coughing. I thought “that was strange.” Thereafter, I noticed that candy and high sugar seemed to cause me to cough. It slowed me down some, but didn’t stop me.
As I reach early adulthood I did what most American bachelors do. I skipped breakfast as I high tailed it to work. I ate fast food and restaurant meals for lunches and dinners. This highly processed, high sugar diet coupled with a long list of stress factors are the risk factors that led to the onset of my acid reflux.
By the way, my 15 years of suffering acid reflux has left me with a lot of stories. Many of them quite embarrassing, but I have chosen to share them in detail in my book:
Connect With Me
 Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
This content is for informational purposes only and is not medical advice. Consult your physician for personalized care.
This free site uses affiliate links. If it's helpful, consider purchasing using the product links —I earn a small commission at no extra cost to you.
Triggers
Before we delve deeper into the topic of risk factors, I need to draw a distinction between triggers and risk factors. Most acid reflux sufferers are intimately familiar with the topic of triggers. These are (most often) food or drink items that will initiate a near immediate / negative response in the body which is accompanied by the escalation of existing acid reflux symptoms.
The list is wide and includes things like mints, chocolate, spice, tomatoes, etc. For me, when my body temperature reached a certain level I would explode into a coughing hacking fit. I could almost feel my stomach contents rising with the temperature until they just boiled over in a flash. This is an example of a non-food trigger that I later pinned down as a side effect of long term acid reflux medication use. That said, some of the more common food based risk factors are shown in the below chart:

Risk Factors
So a trigger escalates the frequency and severity of an existing disease. In contrast a risk factor is a set of conditions that, when present, increases the likelihood of a disease occurring in the first place. That said, I tend to think of risk factors in terms of three categories. These are medical, disease, and lifestyle factors.
Furthermore, these risk factors can affect aspects of the underlying disease in a number of ways. To that point, I have further categorized some of the common risk factors according to their effect on the body’s ability to keep food contained in the stomach, digestion, and lastly the ability to efficiently move food contents along the digestive tract.
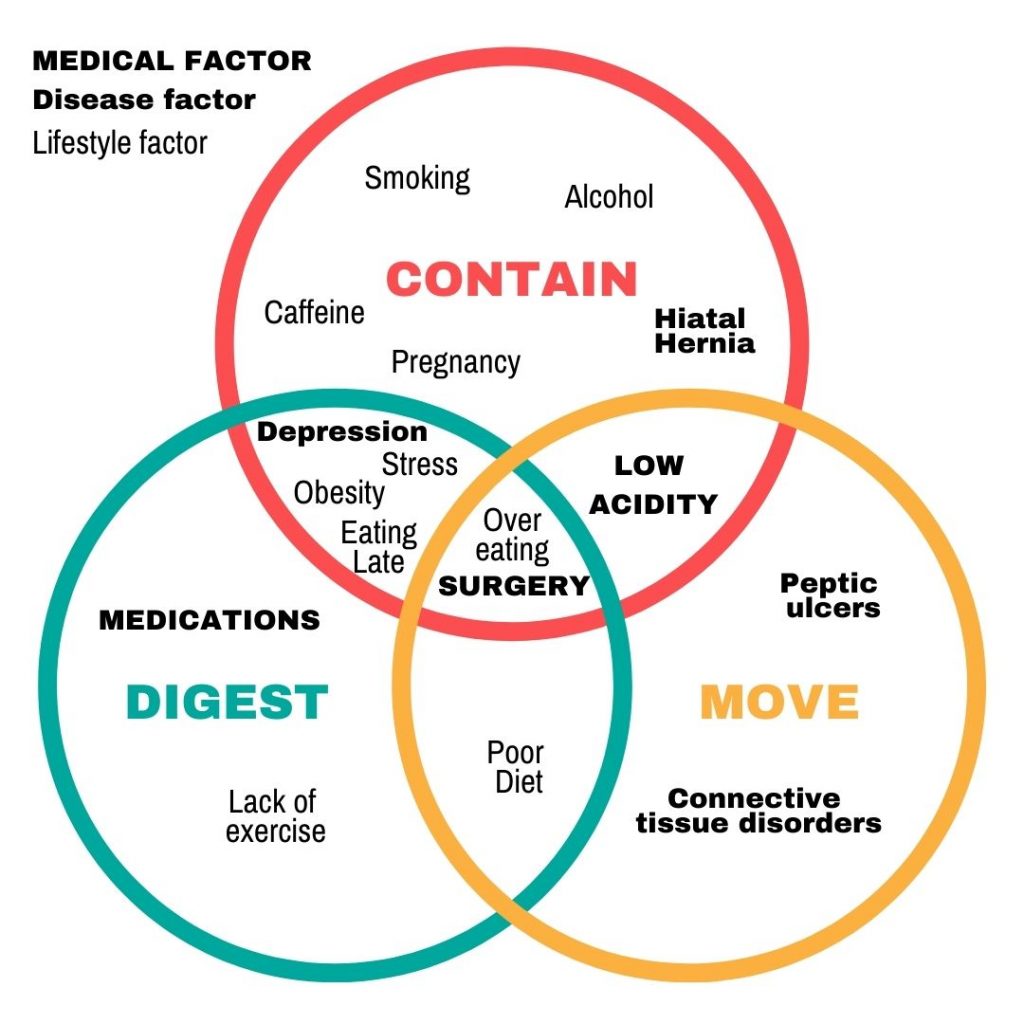
Quick note: If you haven’t already, you need to read my ‘How I Cured My Silent Reflux‘ article, as I write a length about the body’s 5 anti-reflux barriers. This and my coverage of the microbiome are important context for understanding the why below topics. Go ahead and read that article and then come back to this one. It will make more sense.
As I look at the above chart, one thing I find really interesting is that overwhelmingly the lifestyle factors seem to have a direct impact on the body’s ability to keep stomach contents contained in the stomach (indigestion / regurgitation). As covered in above-linked article, this stems from microbial imbalance in the gut and the loss of control of your lower esophageal and pyloric sphincters.
Also in this chart, notice how many of these risk factors are related to poor eating habits such as eating late, over eating, poor diet, and obesity. As we covered in the aforementioned article, a narrow, highly processed, and/or high sugar diet (typical American diet) can drive imbalances in the microbiome and lead to a whole host of disorders including acid reflux. Persistent stress and depression have been shown to have a similar effect on your gut flora as persistent stress has been shown to directly and detrimentally impact microbiome health. Furthermore, the digestive process is inadequately engaged if you are not in a parasympathetic (calm and ready for digestion vs stressed) state when eating.
I want to comment on some of the medical factors. For instance, antibiotics are designed to kill harmful bacteria. Unfortunately however, medical science is not so precise as to have the ability to target and kill a specific strain of bacteria. Instead, these antibiotics kill a wide spectrum of microbes, including the beneficial varieties which makes room for less desirable pathogens to further colonize your gut.. Also, surgery is a common risk factor. This, as your body is thrust into a state of stress while the body heals, you commonly take a cocktail of medications in preparation, during, and after the procedure to fight infection. As with a long list of commonly prescribed medications (including those for asthma, blood pressure, depression, sedatives, antidepressants, narcotics, tranquilizers, antibiotics, acid reflux, etc), these compounds can be harmful to the microbiome and drive imbalance.
I want to make special note of the last class of medications on the aforementioned list (acid reflux medications). At the outset of this article we noted the irony of taking digestion (acid) suppressing medications to treat a disease that is inherently driven by poor digestion. Sadly, the issues do not stop at irony. As covered in the How I Cured My Silent Reflux article, the damage caused by these medications is far reaching from disrupting gut motility (movement of food), to the anti-reflux barrier, to driving microbial imbalance that erodes the gut lining, destroys digestion, reduces immunity, creates inflammation, induces malabsorption of nutrients, encourages infection, and more. Some of the aforementioned risk factors can start the fire of acid reflux, but in many ways these acid suppressing medications pour in fuel and fan the flames.
Lastly, I want to mention the hiatal hernia. This one is a bit personal for me, as I was diagnosed with a hiatal hernia now more than 8 years go. I remember heading into the procedure with mixed emotions, as after 7 years dealing with acid reflux I was receiving my first actual diagnostic and had hopes of getting some answers that might lead to better management or even eliminating my reflux. At the same time, it was a procedure where I would have to go under general anesthesia (sleeping medication) while they stuck a small / camera down my throat to see inside. My doctors also informed me that they would be looking for polyps, which are small growths that are common side effects of acid reflux medication. One or two would be lanced and the tissue would be sent to the lab for biopsy (cancer screening).
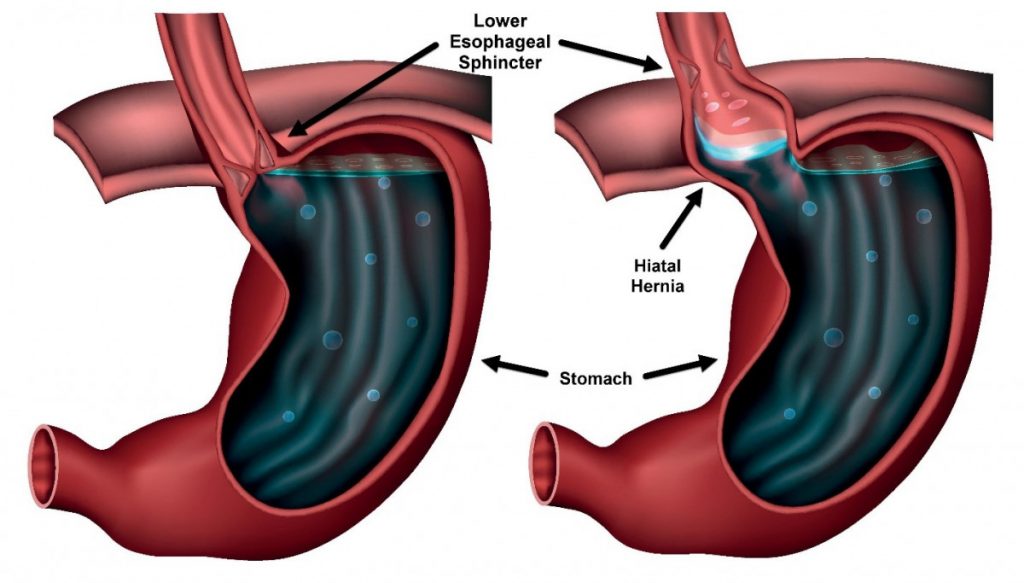
The procedure itself is quick and painless (less than 20 minutes) and my wife drove me home. My doctor later called me with my results. Thankfully, while my stomach was littered with polyps they did not find signs of cancer. I have not had a follow up and the prospect of stomach cancer still remains a daunting possibility in my future. The procedure also identified that I have a hiatal hernia, which my doctor promptly informed me was the root cause of my reflux. For the doctors this was case closed. For me, this was a life sentence for acid reflux, meaning I would suffer the medications and symptoms of reflux for life.
Now, many years later, having beat acid reflux, and having studied it extensively I know that hiatal hernias are actually quite common. Johns Hopkins explains that less than 10% of those with hiatal hernias experience any symptoms. This means, there are most likely other risk factors involved. In fact, it is a bit of a red herring as most people with them do not suffer any reflux symptoms. I want to be careful here as I don’t want to leave you with the impression that all hiatal hernias are made alike. On the contrary, I just want to give you hope if you are dealing with a hiatal hernia, that your condition may still be treatable as mine was.
Summary
In this article, we have covered the common risk factors that can lead to the onset of acid reflux disease. I hope sincerely that this information will help you greatly on your personal journey to eliminate this terrible disease! Your learning does not have to end here. In fact, I would encourage you to get my Amazon #1 Best Selling Book that provides a three phase plan to recovering form acid reflux.
Lastly, I am on a mission to positively impact 100,000 people this year. If I have inspired, helped, informed or otherwise assisted you in anyway, let me know by giving me a follow on any of the below platforms or join my mailing list. If I have yet to do so, then take advantage of the daily tips available on these sites!
 Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
Don Daniels
Latest posts by Don Daniels (see all)
- Honest Review: Wheat Belly by Dr. William Davis - July 10, 2025
- GERD but No Heartburn: Critical Clues Doctors Miss - May 24, 2025
- Feels Like Something Is Stuck In My Throat? Discover Why - May 23, 2025



