In this post we will cover the following topics:
Silent Reflux Disease
As the name suggests there are some differences between silent reflux, acid reflux, and GERD. Namely, silent reflux does not typically cause heartburn. Symptoms commonly include:
- Hoarseness, inflammation of the throat and vocal chords
- Excessive throat clearing and coughing
- Mucus production and post nasal drip

As indicated in the Annals of Clinical Case Reports silent reflux has many synonyms including:
1. Extraesophageal Reflux
2. Supraesophageal Reflux
3. Gastropharyngeal Reflux
4. Atypical Reflux
5. Pharyngoesophageal Reflux
6. GERD Cough
7. Laryngopharyngeal Reflux (LPR)
That said, Silent reflux is most commonly referred to as LPR.
Silent Reflux Symptoms
In addition to the more common symptoms listed above, the following complications can manifest in cases of extended silent reflux.
- Hoarseness / Pain When Speaking – A hoarse voice is often one of the first symptoms that LPR sufferers experience. This, as the larynx (voice box) is very close to the esophagus and consequently has higher exposure to potential reflux.
- Bad Breath / Bitter Taste In Back of Throat – Iron, bitter or sour taste in the mouth is due to stomach contents re fluxing into the airways and mouth.
- Stress – Stress, like anxiety are both side effects of social pressures and reflux medications.
- Burning / Dry throat – Throat pain is one of the earliest warning signs of reflux as the vocal chords and the larynx (throat) are the closest organs to the stomach.
- Excessive Belching – Copious burping goes hand in hand with silent reflux, as frequent exposure stomach gases is the cause of the vocal chord damage and burning sensations in the esophagus and mouth.
- Breathing disorders – Such as apnea, noisy breathing, pauses in breathing, or Choking Episodes (especially at night).
- Asthma-Like Symptoms – Asthma is a common initial misdiagnosis, this is because stomach contents aspirate into the airways, prompting an immune response that mimics asthma
- Ear infections – The ear, nose, and throat are all connected so inflammation, bacteria, and mucous responses can express through any of the three organs.
- Chronic Cough and Throat Clearing – Often times this can be a non-productive cough. LPR can irritate your mucus membranes which can also stimulate coughing and throat clearing. Quite often, silent reflux sufferers are mis-diagnosed as having another respiratory disease like asthma or sleep apnea.
- Globus Syndrome – This is that all too familiar sensation of something stuck in your throat. This is due to inflammation and swelling of your membranes.
- Difficulties swallowing (dysphagia) – Many LPR sufferers experience trouble swallowing due to throat inflammation.
- Post Nasal Drip – Post nasal drip and mucous production is your body’s natural response to protect sensitive tissues in your nasal cavity and esophagus (throat) from acid and acid vapors. This can result in excessive mucus in your throat and airways.
- Nausea or vomitting – This can be a side effect of throat stimulation or digestive issues, which ultimately may be the source of your reflux issues.
- Frequent Infections – As acid reflux is most often a symptom of poor digestive health and low stomach acidity. In a low acid environment, pathogens (such as bacteria and viruses) are able to thrive.
- Anxiety – Anxiety is often two fold 1. social stigmas from bad breath or hoarse / muted voice and 2. a side effect of vitamin B12 deficiency, a common side effect of long term acid reflux medication usage.

Take The Silent Reflux Quiz
To Heal, You Need To Address The Cause Of Your Reflux
Endless guidance and advice exists on the internet to help you eliminate your acid reflux, ranging from jaw exercise routines to diet plans. While some are helpful, most including prescription medications, focus on managing or reducing the discomfort caused by your symptoms. They do little-to-nothing to resolve reflux because they fail to address the actual root causes of the disease.
To put this in context, Americans spend more on their annual subscription to prescription acid reflux medications than they do on some video streaming services ($10 Billion on Proton Pump Inhibitors vs $2 Billion on Hulu Streaming Services). Yet, while the symptoms are somewhat alleviated, the disease remains. In fact, the disease tends to escalate in severity and frequency over time. This is because, at best, these medications only treat the symptom not the cause.
This is a topic that I am quite passionate about because I suffered with reflux for more than 15 years. Over that time I contributed to the $10 Billion as I estimate spending over $6,000 on prescriptions, over the counter medications, and antacids. Like you, I became increasingly dissatisfied with medical advice. However, with my hiatal hernia I was resigned to the fact that I would suffer the disease for life. Furthermore, my doctor essentially said my options were a lifetime prescription or throat cancer, as surgical technology still does not offer a long time solution.
However, for me everything changed when my symptoms suddenly took a turn for the worst. After eating a handful of candy at work I added several new and excruciating symptoms (persistent burning / sour mucus, post nasal drip, constant burning in the roof of my mouth and lips) that would plague me for the next 6 months, and that motivated me to understand address the root causes of my reflux and eliminate it for good.
The amazing thing is remedies such as the one described in this article are relatively simple, fast, and inexpensive. Sadly, however they are little known because the concepts are partially based on science that is only twenty years old, are somewhat counterintuitive, and contradict millennia of cultural understanding on this topic.
For thousands of years, a home remedy for indigestion involved chewing chalks and food grade charcoals. In modern day, these naturally occurring compounds (such as calcium carbonate) are the active ingredient in popular antacids such as Tums, Alka Seltzer and Pepto Bismol.
In addition to the long history in our culture around the concepts of acid suppression, the prevalence of acid blocking medications, the power of the pharmaceutical advertising machine, and the institutionalization of these medications easily crowd out more modern, targeted, and effective approaches to dealing with the disease.
If You Have Reflux, Here Is Why
There are two principle root causes for acid reflux. The first is a microbial imbalance in the digestive tract. The second is low acidity. In this section we will touch on both. Be sure to read to the end, however as we will also cover common risk factors that may have led to the onset of these root causes as well as the many strange side effects and symptoms of long term acid reflux that you may not have attributed to the disease.
Microbial Imbalance In the Digestive Tract
Have you ever had a feeling of butterflies in your stomach when you were doing something new, risky, or scary? That is because the gut and brain communicate with each other and are intricately connected. In fact, over the last twenty years a whole new field of medical science has emerged around this topic, called the gut-brain axis. Astonishingly, the gut which is often referred to as the second brain, has more than 500 million neurons. As you may know, the neuron is the fundamental unit of the brain and is responsible for interpreting sensory input and sending motor commands to the body.
What we have since learned is a third and equally important component of this connection called the microbiome. Your microbiome is the 5 pounds (2.3 kilos) of microorganisms and genes that live in your body and are essential to your survival. In fact, this expanded field of study which is now referred to the gut-brain-microbiome axis reveals that the number of cells in your microbiome outnumber the human cells in your body by a factor of 10-1. In fact, there are more than 100 trillion microorganisms including bacteria, fungi, viruses, and protozoa in a healthy human body.
We know the most about the 1000 species, and 7-9000 strains of bacteria because many of them can be cultured and studied in a laboratory environment. Much like the numerous examples we see in nature (Egyptian Plover removes rotting flesh from the open mouth of a Crocodile, Clownfish provides nutrients and the Sea Anemone provides protection) of co-operative organisms, they symbiotic bond with their host. Even more surprising, similar to the recently discovered co-operation and communication between trees via fungal networks, the gut, brain, and microbiome share three way communication.
We are only beginning to understand the depths of connection between this triumvirate. But, through study of mice and application in humans via Functional Medicine we know that a balanced microbiome is key to a healthy immune system, digestion, production and absorption of vitamins and nutrients, production of hormones such as dopamine (essential for brain and nervous system function), serotonin (mood and wellbeing), melatonin (sleep), adrenaline, and more. Full coverage on this and other topics are beyond the scope of this article. That said, I have expanded on it in my recently released book:
Needless to say, I could easily start a series by authoring second title devoted to this topic. The key thing you need to know is an imbalance in the microbes that colonize your intestinal tract can be catastrophic to not only your digestion, but your mood, nervous system function, immune system, nutrition, brain health, and more. There are many risk factors that can lead to this imbalance, that we will explore later in the article. For now, we will explore a few of the more significant side effects of this this bacterial imbalance, also known as dysbiosis.
Feel like you've done all the things and are just not seeing progress? I've helped a lot of people over the years that felt the same way. Perhaps an at home microbiome test can help break the cycle and provide the insights you need to move froward. With it, you can test your gut microbiome and receive actionable recommendations on how to optimize your digestive health with the BIOHM Gut Report.
I have arranged a 20% discount if you use the code THEACIDREFLUXGUY at checkout!
Indigestion
I start with indigestion because it is perhaps the earliest and most direct impact of dysbiosis. Your gut microbiome is considered ‘unbalanced’ when the proportion of beneficial microbes is outnumbered by their harmful counterparts. When in low numbers, these microbes are often harmless and can even be beneficial (more than 50% of people, in fact, have H Pylori). In fact, recent studies such as this one by Harvard Health indicate that H Pylori, often attributed for the development of Irritable Bowel Syndrome (IBS) may actually play an important role in regulating stomach acid.
That said, the wrong bacteria such as H Pylori or Clostridium Difficile (C. Diff.) can grow out of proportion in your stomach. For some of these bacteria, the process of decomposing food leads to fermentation and excess gas production which causes bloating (a common reflux symptom). Normally, this fermentation process should occur in the colon where it can be expressed through the anus. However, under the wrong conditions bacteria that normally colonize the colon are allowed to proliferate in the gut.
Additionally, as we have discussed, your body depends on the symbiotic relationship with your microbiome for digestion. When unbalanced, food contents sit on your stomach for extended periods, leading to indigestion (another common reflux symptom). As this occurs more often, this creates a cycle that supports further colonization of the offending bacteria, which in turn leads to higher frequency and severity of indigestion.
Impaired Immune Function
Another important function of your microbiome is to improve immune function. Amazingly 70-80% of your immune cells are found in your gut. This might seem surprising at first, but think of it this way: We like to think the only portion of our body that is exposed to the outside world is our skin. But there is no dividing line between your skin, down through your mouth, throat, stomach, intestines, and colon; it’s all connected!
Additionally, your skin has an estimated surface area of 2 square meters which pales in comparison to the estimated 30 square meters of your digestive tract. By surface area, your digestive tract is WAY more exposed. Understanding this, the foods and drinks that you put into your body pose a more significant threat as compared to viruses and bacteria that are exposed to your skin.
One way your microbiome aids your body’s immune system is by helping to efficiently digest foods and prepare them for movement down the digestive tract. Foods that sit on the stomach too long or that are poorly digested can lead to inflammation, which can compromise the stomachs mucosal lining. In fact, when the body is unable to process a food it is tagged as an invader and attacked by the immune system, which triggers an inflammatory response. Inflammation allows the body to trap the offending agents so the immune system can consolidate an attack.
This inflammation is fine in isolated events, but the persistent presence of poorly digested foods leads to chronic inflammation and long term damage of the single cell thick lining of the stomach. This occurs more often as bacteria are further out of balance as more and more foods cause and inflammatory (or triggering response using acid reflux terminology). Ultimately damage to the stomach lining (known as leaky gut) can allow for food particles, and harmful pathogens to enter the blood stream. This leads to inflammation in other parts of the body, such as the brain, which leads to brain fog, memory issues, anxiety, etc.. As you will see in the risk factors section, this can contribute to the downward spiral and ever escalating situation that characterizes acid reflux.
Malnutrition
Lastly, I’ll cover malnutrition. As with any symbiotic relationship, neither party is altruistic! We humans get a needed boost to literally every body function, as proper digestion leads to the extraction of energy in the form of amino acids, simple sugars, fatty acids, etc. These ultimately form the building blocks that make us, us! The microbiota get the nutrients that fuel their incredibly short, yet productive lives.
Amazingly, a healthy gut, brain, and microbiome are in constant communication and coordination with regards to the production of building blocks for healing, immune function, proper cell function, development and conversion of hormones, etc. For instance, the human body alone is incapable of regulating estrogen levels, an essential hormone for women’s health. In fact, it is your microbiota that create the beta-glucuronidase that converts estrogen into its active forms.
As you can imagine, when these biota are imbalanced it can lead to a number of physical and neurological disorders. The brain, for instance is primarily composed of fat. Absent the abundance of critical building block our minds are quite literally limited. This can manifest due to malabsorption but also because certain bacteria are highly efficient at leeching certain nutrients for themselves.
Do you ever feel like all your food is out to get you? No surprise, when medical world's answer to reflux is blocking digestion (acid blockers). Wouldn't it be nice to enjoy more of the foods and drinks you love, with less of the indigestion?
I know because I was were you are for more than 15 years. That's why I created Digestion Transformation Checklist. In it, you'll find 19 actionable tips to boost your digestion, from the start to finish.
Ready for some relief? Just enter your details in below, and get the guide straight to your inbox for FREE!
Low Stomach Acid
Paradoxically, the other leading root cause of acid reflux is low stomach acid. You read that correctly, it is not high, but LOW stomach acid that often leads to acid reflux. There are many reasons for this. The first, and perhaps most obvious is the fact that reduced stomach acid impairs digestive efficiency which leads to indigestion. High stomach acid is required to efficiently dissolve your foods and prepare them for further digestion as it passes along the gastrointestinal tract.
Additionally, stomach acid is required as a signaling mechanism for the body to perform certain digestive and anti-reflux functions. In fact, the body is designed with five anti-reflux mechanisms that are controlled through the gut-brain-microbiome axis via the vagal nerve, which serves as a communication super highway. This nerve is the longest in the human body and a pillar of the autonomic nervous system. It alone conveys 80-90% of the body’s sensory information concerning the state of the body’s organs.
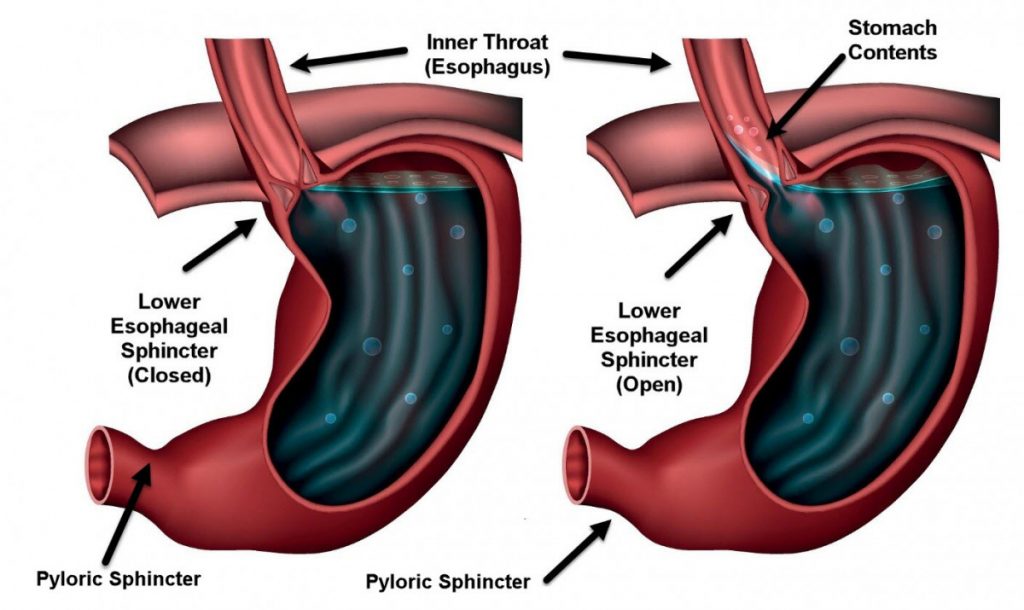
The first three anti-reflux / digestive mechanisms are the lower esophageal sphincter (LES), diaphragmatic sphincter and pyloric sphincter. Sphincters are a common design pattern in the body and exist as a ring shaped muscle that controls the passage of solids, liquids, and gases. Some are under voluntary control such as the anal sphincter (allows you to poop), the upper esophageal sphincter (allows you to swallow / burp), and the urethral sphincter (allows you to pee). In contrast, the LES, diaphragmatic and pyloric sphincters (pictured below) are signaled to open / close through your vagus nerve as a response to acidity.
The pyloric sphincter is responsible for emptying stomach contents into the lower intestines once sufficiently digested. If acidity is too low, signaling to the brain is weak or poorly timed, which leads to delayed digestion (indigestion) and bloating. The LES and diaphragmatic sphincters are responsible for keeping stomach contents out of the throat. If acidity is too low, these muscles do not contract with sufficient pressure and will allow stomach contents to flow backward into the throat.
The other two anti-reflux mechanisms are a bicarbonate (antacid solution) that is produced in your throat and saliva. This occurs automatically as well as a response to acid and levels of natural antacid can actually increase as much as 32 fold. This is the body’s last line of defense however and the low grade antacid are in sufficient to handle the high levels of stomach acidity that enter the throat and mouth due to poor sphincter function and indigestion.
Lastly, on the topic of low stomach acid I want to mention the fact that the stomach is designed as a highly acidic environment. In fact, as a measure of acidity from 1-14pH, with the highest levels expressed in low numbers, stomach acid is naturally in the range of 1-3 pH. This is slightly less potent than battery acid! Normally, the stomach, its mucosal lining, and your anti-reflux barriers are more than a match for this highly corrosive environment. It is necessary for digestion, to kill harmful pathogens in support of your immune system, and to support healthy balance of gut bacteria. For this reason, it is quite often that Small Intestinal Bacteria Overgrowth (SIBO) or Irritable Bowel Syndrome (IBS) often accompany low stomach acid.
Connect With Me
 Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
This content is for informational purposes only and is not medical advice. Consult your physician for personalized care.
This free site uses affiliate links. If it's helpful, consider purchasing using the product links —I earn a small commission at no extra cost to you.
How I Cured My Silent Reflux
Many people who contact me come armed with a dozen or more things that they’ve tried in attempts to eliminate their reflux. The problem is very few of these supposed solutions can be correlated back to a root cause issue that they help resolve. Some do help to mitigate symptoms, but they do not offer healing. Sadly others like Gaviscon worsen symptoms because they reinforce the root causes by lowering acidity. Many are surprised by this as they were only aware of the highly advertised foam barrier that it purports. If I had a dollar for every time I heard the word Gaviscon from one of you I could easily cover the cost of maintaining this website!
Sadly, people are lulled into believing these medicines are helping them because they neutralize the uncomfortable / painful acids that escape into the throat. Consequently they decide to take them longer than the recommended 6-8 weeks, and because doctors do not have a better alternative they suggest buying over the counter or renew the prescriptions.
That said, I want to cover some of the more serious effects of long term acid reflux medication usage. It is well documented that long term use leads to several vitamin deficiencies, namely vitamin b12, magnesium, and calcium. Below is a list of the most common side effects. If have bolded several that I personally dealt with for years, not realizing they were associated with reflux. If you have experienced any of the below, you may be deficient in one or more of these vitamins.
- Weakness, tiredness, or lightheadedness
- Heart palpitations and shortness of breath
- Pale skin
- A smooth tongue
- Constipation, diarrhea, loss of appetite, or gas
- Nerve problems like numbness, muscle weakness, and problems walking
- Vision loss
- Mental problems like depression, memory loss, or behavioral changes
- Muscle Problems (aches, cramps, spasms, numbness, tingling in hands, arms, feet, legs and around the mouth)
- Extreme fatigue
- Nail and skin symptoms (itch, inflammation, psoriasis)
- Osteopenia and osteoporosis (low bone density)
- Painful PMS
- Dental problems
- Nausea
- Loss of appetite
- Anxiety
Now, with your understanding of the root causes and long term side effects of reflux, I hope you are in a better position to judge the potential efficacy of the potential treatments that you try, before you spend time and money on them. As reflux is a multi-pronged issue, including digestion issues, microbial imbalance, malabsorption, and low acidity the solution needs to be one that addresses all of these issues. An effective approach should provide short term relief sufficient to enable a transition away from existing medications as well as a long term foundation for continued healing.
As such, I have summarized an approach that I used to successfully transition off of my acid reflux medications and ultimately to eliminate my reflux entirely.
Revise Phase I (2 weeks): Create a stable digestive environment to enable a smooth transition
- Avoid common and and identify your personal trigger foods
- Add naturally fermented foods to your diet (for probiotics)
- Add high fiber foods to your diet (prebiotics) to rebalance your gut
- Take b12 and magnesium supplements (if you are deficient)
Restore Phase II (4-6 weeks): Supplement digestion & transition off reflux medications
- Take apple cider vinegar capsules (not liquid as it is corrosive) for prebiotics and to kill harmful pathogens
- Use digestive enzymes with meals to improve digestion
- Take betaine hydrochloride with pepsins with meals to restore acidity and sphincter function
- Stop taking reflux medications
Renew Phase III (2+ weeks): Reintroduce foods
- Slowly Reintroduce foods
- Avoid risk factors to avoid re-entering the reflux cycle
 For a comprehensive / easy to follow plan, additional rationale, and the steps I took to resolve my reflux, get my #1 best-selling book 'How I Cured My Silent Reflux | The Counterintuitive Path to Healing Acid Reflux, GERD, and Silent Reflux (LPR).' Also available in audiobook!
For a comprehensive / easy to follow plan, additional rationale, and the steps I took to resolve my reflux, get my #1 best-selling book 'How I Cured My Silent Reflux | The Counterintuitive Path to Healing Acid Reflux, GERD, and Silent Reflux (LPR).' Also available in audiobook!
Risk Factors
Lastly, I want to briefly cover the three categories of risk factors that you should be aware of. This may help you correlate the onset of your symptoms to a lifestyle, disease, or medical event. This is important so that you are able to avoid falling back into the reflux cycle after you may have healed:
- Lifestyle Factors: Smoking, Alcohol, Caffeine, Pregnancy, Stress, Obesity, Eating Late, Over Eating, Poor Diet, Lack of Exercise
- Disease Factors: Hiatal Hernia, Peptic Ulcers, Connective Tissue Disorders
- Medical Factors: Surgery, Low Acidity, Medications (Asthma, Blood Pressure, Depression Medications, Sedatives, Antidepressants, Narcotics, Tranquilizers, …)
These are by no means an exhaustive list, and I go into more detail on these topics in my book, as well as ways each can affect the body’s ability to keep stomach contents contained, efficiently digest, and affect movement of food contents along the digestive tract.
For instance, I’m sure you know that exercise positively affects metabolism, but did you know It also directly effects digestive health and efficiency? This is achieved through a process called peristalsis, which moves food along the digestive tract through a series of involuntary yet coordinated muscle movements.
Also, the content of your diet has a direct effect on digestive health. The more narrow, processed, and high in sugar your food choices are, the more your digestive system is skewed to process these foods. This leads to harmful imbalances and side effects that negatively affect digestive efficiency.
Summary
In this article, we have covered silent reflux, its symptoms, and root causes as well as the treatment protocol that I applied to eliminate my reflux. I hope sincerely that this information will help you greatly on your personal journey to eliminate this terrible disease!
Lastly, I am on a mission to positively impact 100,000 people this year. If I have inspired, helped, informed or otherwise assisted you in anyway, let me know by giving me a follow on any of the below platforms or join my mailing list. If I have yet to do so, then take advantage of the daily tips available on these sites!
 Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
Take advantage of my daily tips on Instagram, YouTube, or join my mailing list to learn how hundreds, just like you, have taken control of their health!
Don Daniels
Latest posts by Don Daniels (see all)
- Honest Review: Wheat Belly by Dr. William Davis - July 10, 2025
- GERD but No Heartburn: Critical Clues Doctors Miss - May 24, 2025
- Feels Like Something Is Stuck In My Throat? Discover Why - May 23, 2025





I want to report that this solution WORKS. I have been having all the silent reflux symptoms for several months – no heartburn yet cough, lump in throat/hard to swallow, post nasal drip & congestion, and especially tons of saliva that kept accumulating in my mouth. I had to swallow every 5 seconds. Well, I thought it was saliva. I guess it was the mucus! After $2,000 and 3 ENT’s, who gave me the PPI’s which didn’t work, I tried the ACV and Betain supplements before eating. At first, I only took one of the ACV tablets but after a… Read more »
Laura, I’m so happy to hear you’re beginning to feel better 🙂
Don
I just knew that I was going to get the bottom of this article and find that you were selling something instead of offering tangible, informative and useful information. I don’t quite have the words to express how grateful I am for your willingness to share this information. I have been battling with LRP for roughly two years and entirely without medication because I refused it. What I have had is bits and pieces of information to assist but never a real concrete plan for healing. You have no idea the amount of hope you just offered me. I’m only… Read more »
Hi Tamera, Sorry for the late reply. For some reason I didnt receive a notification. You are very welcome. Hope you are able to find healing soon 🙂
Best Regards,
Don
Don, I just wanted to thank you for putting this information out here for all of us! I took my 17 year old son to see his ENT for the same cough that he gets consistently. Luckily, I already knew walking into his office, that it was from acid reflux. Doc did the scope and confirmed, yep, totally acid reflux and prescribed the drugs. Really? He’s 17! I was not going to start him on a drug that he would have to take on and off for the rest of his life. I started my son on the supplements and… Read more »
Hi Francine, Thank you so much for your post and for sharing this wonderful news! Congrats on your son’s speedy recovery 🙂
Don
What do you consider naturally fermented foods? And thank you for this information
Another question. If pepsin is what’s causing the sore throats where it is embedded in the throat. How is it safe to take a supplement with pepsin. And do you recommend DGL?
Hey Ben, Most modern store-bought pickles skip real fermentation altogether, so if you’re trying to include dill pickles as a fermented food source, you’ll need to look specifically for ones that say they’re naturally fermented (often they’re in the refrigerated section, in brine, not vinegar). Beyond pickles, other fermented foods like sauerkraut or kimchi are usually true ferments, but always double-check the label. Just keep in mind: fermented foods can be quite acidic, so if you’re dealing with throat irritation or inflammation, they might make things worse for a while — especially if you’re already healing damage. About the pepsin… Read more »
Hi I am from India suffered a lot by silent reflux i don’t know it’s a silent reflux.severe burning sensation in my throat feel horseness in my voice want to expel every 10 min from my throat slight burning sensation in my chest area.Today only i started apple cider vinegar with 3 betaine hcl.can I take kefir for my probiotics
Thank you for this great information. I have suddenly been beset by LPR and a horrific case of globus sensation. Your protocol seems very aligned with the protocol I am using with my naturopath to address this. However I can say that after three weeks of attempting to do the natural approach, with the globus sensation the only thing that gives me relief is Gaviscon – which I am only taking once each day, just before bed when the pressure in my throat is intolerable. This puts me in a bind because I know Gaviscon is reducing vital stomach acid… Read more »
Hi Elle, You may need to identify acidic foods in your diet, anything that is a 1-5 pH (measure of acidity). That or work to minimize nocturnal reflux, if that’s something you’re dealing with as it may be adding inflammation to your throat (source of the lump feeling). This section of the blog may help: https://theacidrefluxguy.com/root-causes-real-answers/#acid-reflux-triggers
Best Regards,
Don
Thank you for this highly detailed post. I fixed my low stomach acid (accidentally) with apple cider vinegar with “Mother” in it. Glad others are turning to natural remedies to fix stuff that doctors will shove prescriptions on!
How did you come off of your PPIs? Gradually or cold turkey? How did you handle rebound? In reading your book and how you got rid of reflux, you say to stay on reflux medication for phase 1, but to stop with phase 2. This is so confusing to me.
Hi Carol, The phase 2 supplements confined with the dietary modifications controlled the rebound symptoms. When the body has sufficient acidity and is able to digest properly, indigestion doesn’t occur but more importantly, the lower esophageal and pyloric sphincters which open and close in response to acidity and intraabdominal pressure are signaled to close
Hi Don. I’m just about there! I still get gas in my throat if I bend down or if I haven’t eaten for approximately two hours. Not sure if I’m taking enough BETAINE. What do you suggest
Hi Leeann, hard to say with limited information, but I have a betaine hcl playlist that might help: https://www.youtube.com/watch?v=2ItHnmG3Mso&list=PLZlZsM0_MFmk_4ep3oHdp5fGp4DqwQKW8
Hi can you have Greek yoghurt instead of plain yogurt?
Most definitely!
Dear Don, First of all I would really like to thank you for sharing this article. After having visited an ENT specialist, and a Gastroenterologist (several times), I am still suffering from severe heartburn as well as burning mouth and throat + teeth sensitivity. I was prescribed PPIs and ant-acids for immediate relief but these have not been really working for me either. I would like to ask you something with regards to the supplements. I have found these from Holland and Barrett. Do you think they are ok? Holland & Barrett MultiDigestive Enzyme 90 TabletsHolland & Barrett Apple Cider… Read more »
Hi Andrew, Sorry for the late reply. For some reason I didnt receive a notification of your comment on the site. The apple cider vinegar looks fine, though a bit lower dose than I used (500mg). The only real issue I see is that the digestive enzymes are combined with the HCl and the HCl is in low dose (100mg). This may make it difficult to adjust your HCl dose. For that reason, I prefer them seperate.
Best Regards,
Don
Dear Don, Many thanks for you prompt reply. Unfortunately symptoms have worsened. I too have a hiatus hernia which is supposedly small but the symptoms are far from small. I started having severe burning sensations in my mouth (I also have very bad heartburn), very sensitive teeth, and the buccal mucosa especially at the back has started to break. Needless to say I am in severe pain. I have had to start treatment with PPIs once more after having failed with trying out natural supplements. DId you also have any of the above mentioned symptoms? (The mouth ones) Would really appreciate… Read more »
Hi Don! After not getting proper sleep for the past two months (drainage and coughing at night, which I assumed was allergy related) I made an appointment with my ENT. He asked a few questions and checked with an endoscope, discovered that I have LPR. Started on Pantoprazole 40mg 11 days ago, but decided that I needed to do more research and found you!! I couldn’t wait for your book to arrive from Amazon, so I got the audio version and took notes! Wow! I am so grateful to you! I have a follow up appointment with the ENT in… Read more »
Hi Karen, Thank you so much for the kind words. I sincerely hope that the book is helpful for you :). From what you describe, it doesn’t seem the Pantoprazole is managing your symptoms at all. If that’s the case and knowing the side effects, I personally would look to get off of them.
Best Regards,
Don
Thanks Don! Really, I can’t thank you enough for your help!
Karen
My Doctor said I have LPR Reflux. In February I had a full thyroidectomy due to the fact that I had an enlarged goiter and problems with nodules. I am taking Dexilant for the LPR Reflux due to the fact that I have the mucus in the throat, sometimes it’s hard to swallow certain foods and medication. I am taking vitamin D3 and getting a B12 shot must months, but still having these problems. This is so frustrating – what were the supplements you recommend. I trying the wipeout diet, but look like LPR still problem.
Hi Sandra, Thanks for your question and sorry to hear what you have been going through. Let me provide you a shortcut to a few resources. I list the supplements that I used on my resources page. These are part of a holistic plan that I have detailed in my book
Hope that helps,
Don
Hi Don, further to my 1 comment, I have breathing issues mostly at night which are on & off, I’m not able to get sleep at night coz of this I feel really weak.
Hi Don, last month I had a course of antibiotics for ear infection. Ever since I started taking them, I experienced diarrhoea, throat burning, chest pain, back pain, felt like I’m choking at times, throat pain. I’ve taken gaviscon a couple of times. It did not help. I got my blood tested. I have hypothyroidism and also vitamin d deficiency. I’m currently taking thyroid medication and vitamin d3 capsules. I also take probiotics. I still experience throat burn, constant throat clearing, ringing in my ears, and now since yesterday my nose got blocked. I feel terrible. I recently consulted an… Read more »
Hi Reena, I would encourage you to check out Dr Mark Hyman’s YouTube channel. He discusses the links between hypothyroidism, vitamin deficiencies, reflux and gut dysbiosis which was likely further catalyzed by taking antibiotics. He points out that all these issues are linked and if you are able to address the dysbiosis you may be able to address them all. In my book, I discuss the approach I used to resolve my dysbiosis and thereby heal my reflux. What probiotic are you using?
Hi Don, thanks for the valuable information. I take acidophilus plus 2 billion currently just started taking them few days back. Feeling better with digestive issues. But have a burning throat that bothering me since a month now.
A good probiotic certainly helps. Good to hear you are starting to feel better. If you are using the approach in my transition guide or book, hopefully you can see further improvement as your digestion improves.
Best Regards,
Don
Hi there! I’ve struggled with coughing after laughing sometimes severe. Could I have this condition?
Hi Mary, It’s possible, but is that your only reflux symptom?
Throat clearing and a sense of mucous build up. No heartburn that I know of. Sometimes short of breath
Hi Don – as the road to recovery begins, I presume how my throat/voice recovers and how my digestive tract and acidity levels recover – are two different recovery speeds? In using the supplements you suggest, I feel my digestive tract has improved already. I have Silent Reflux, so don’t really suffer from heartburn. But I have had a sore throat/coarse voice and trouble swallowing for 5 months. Does it take time for the throat and voice to revert back to normal? I am sitting with a prescription of PPI’s from the doc. But I am reluctant to start them… Read more »
Hi Ally, Apologies for the delayed response. For some reason, my website doesnt send notifications of comments at times. The bloating and gurgling are signs of a change to your digestive efficiency.
Thank you for your comments and great to hear you’re already feeling a bit better. They are harmless and last 1-2 weeks and then go away. I noticed my voice issues were resolved entirely within two weeks, but as you can imagine there are a lot of variables at play and everyone’s results are unique to them.
Best Regards,
Don
Hi Don, I have been trying some eliminations for the past 3-4 months (no caffeine, chocolate, citrus, high-fat, citrus, onion/garlic etc) alongside other restrictions such as the Acid Watcher diet, low histamine etc, but have had no improvements in my symptoms which I believe to be LPR (post nasal drip, sinus headaches, hoarseness and heartburn) – do you think it is unusual to not see any relief from removing these normal triggers? I am wondering if I need to still continue a similar protocol whilst taking your suggested supplements, even though it does not seem to affect my symptoms. I… Read more »
Hi Sophie, Elimination diet alone is often not enough to eliminate symptoms for a few reasons including 1) residual triggers that may not have been identified (triggers can at times have a delayed reaction of a day or more) 2) persistence of inflammatory / leaky gut issues 3) persistence of dysbiosis that has not yet been corrected, and more. If you have not seen relief from the holistic plan in the transition guide then you may need to ramp up your dietary fiber intake from natural sources (vegetables, fruits, legumes) aiming for 35-50 grams of dietary fiber from these natural… Read more »
Thank you Don, I do already take probiotics (have been for around 2 months) but it does not seem to be helping any of my symptoms. Have you got any good tips for ensuring 35-50g of fibre intake per day?? It is feeling extremely hard to achieve whilst trying to eat small portions so as to not over fill the stomach!
Hi Don, do you recommend any particular brands of the supplements that you suggest? And do you recommend the HCL test to find the right dose?
Hi Jodi, You might consider getting my book , which covers the holistic approach I used to resolve my reflux. Also, the brands I used are all listed on my resources page. Hope you are able to get well soon!
Best Regards,
Don
Hi Don, Thank you for your dedication and for shining light and hope on this misunderstood, and often misdiagnosed, disease. I’ve been chasing answers, and have been misdiagnosed, for over 15 years. I’ve finally come to realize what my doctors and I have thought was adult onset asthma is in fact silent reflux. I have ALL the symptoms, and for the past 2-1/2 years excessive hoarseness and fluid in my lungs has become debilitating. In my research I have encountered alternative accounts as to the source of silent reflux. One of them maintains that it is the digestive enzyme Pepsin,… Read more »
Hi Cris, Thank you for your comment. I don’t have an issue with an alkaline diet (avoiding acidic foods) as a means to avoiding the activation of pepsins. I do have an issue with drinking alkaline water or taking acid suppressers including Gaviscon as they contribute to the reflux cycle (bacterial overgrowth, poor sphincter function, malabsorption, etc..). In these cases we’re trading short term symptom relief for longer term issues that exacerbate symptoms. Rather than address the symptoms, I much prefer focus on addressing the root causes of reflux as described in this article. I would be the first to… Read more »
Excellent job of explaining!
Thank you!
Hi, Don ..1st of all, thank you so much for write it all down. Oh I am so happy to found this post on Pinterest, as I did a lottttt of browsing about what happening & how to get rid of this weirdness in my stomach (if I haven’t eaten or after I am ate😂). I am 43 yo, I had my 1st flare up and did went to ER around 7 years ago (because I thought it was heart attack). And until now, I already went to ER for 3 times and only got a medicine from them (the… Read more »
Don, thank you for this information. After experiencing most of the symptoms you listed for years, I visited a gastroenterologist and I was diagnosed with acid reflux and hiatal hernia. That was about 5 years ago. I was put on Protonix and followed their guidelines as far as diet went. I stopped taking the medication after six months due to the long term side effects you mention. I never got rid of the throat clearing, but figured I would have to live with it. My symptoms got much worse last spring and I started the round of specialists appointments (… Read more »
Hi Linda, You are describing classic symptoms of silent reflux (no heartburn, misdiagnosis as asthma, mucus). There is a survey that you can take that will tell you the likelihood that you have silent reflux. If you would like to take it, you can find it here: https://theacidrefluxguy.com/SilentRefluxQuiz. Also, if needed, I wrote a book with the steps I took to resolve my silent reflux: https://theacidrefluxguy.com/book
Best Regards,
Don
hi Don, a few years ago I hurt my back at work and to keep working and get through the pain I began taking ibuprofen. And I started having heart burn immediately and did for the next few months while I took the ibuprofen.I thought it was safe.. Next thing I know the doctor tells me I may have GERD. I had an upper GI and a colonoscopy. Doc says I also have chronic gastritis…So I have been taking omeprazole since then and changed my diet , but recently I have have too much burping it can go on for… Read more »
Hi Georgie, It is awful that these seemingly harmless drugs like ibuprofen and other anti-inflammatories can lead to inflammatory conditions like gastritis. You may want to consult your physician before taking these as they can potentially aggravate your gastritis.
Best Regards,
Don
Don, I stopped taking the ibuprofen about six months after my injury , when I found out about the harm they do. But it seemed too late.that now I had GERD. Before taking the Advil I had never experienced heartburn my entire life. I haven’t been the same since. My gastro doctor was of no help, after my results came back from upper GI and colonoscopy I had to ask him” so do I have GERD?”and all he said was “probably”and gave me a prescription. He hasn’t helped me at all. Now I have all these other symptoms… ones you… Read more »
Hi Don, I’m happy to have come across your website. I am 30 years old and I have been taking acid reflux tablets on and off since 2007. It got worse last year and I became deficient in vitamins as my stomach is not able to absorb the vital vitamins. I have had a lot of the symptoms you have described. Recently stinging in fingers, constantly clearing my throat and constantly feeling of chest pain. I have started on the supplements you have mentioned but it has not being completely helpful. Especially when I ate sugary food or drinks. Did… Read more »
Hi Teresa, I was careful to avoid triggers early in my transition so that I was more aware of any changes in my body. As the weeks progressed, I had less and less trouble consuming my typical triggers. Even found that I could resume drinking milk (something I had avoided for several years prior). In my experience its not required to eliminate triggers, but helpful to give you the confidence that you are indeed improving.
Best Regards,
Don
Hi Don, My symptoms started this past February at work after eating some dark chocolate at lunch with carbonated mineral water – over the proceeding months things continued to get worse where now every time I eat I have to clear my throat of mucus/cough up mucus/blow my nose. I switched from drinking pop/milk/other beverages with meals to solely water about two years ago and drink pretty much only tap water throughout the day. I went to a naturopath who recommended decolorized aloe vera and that helped after meals, but I tried tapering off after noticing it only worked a… Read more »
Hi Wayne, It sounds as though you have developed silent reflux. Interestingly enough, I can trace the development of severe silent reflux symptoms to a a handful of lifesavers that I ate. Following that the stream of mucus and post nasal drip was seemingly constant. It got worse during and after meals and I found myself getting up from the meal several times to blow my notes. Your symptoms will reduce as you eliminate triggers (chocolate, caffeine, etc..), but in my experience they will not go away without rebooting your digestive system. If you can get things back on track,… Read more »
Apologies for posting another comment, I have additional questions that I didn’t think of in my original one: Is it ok to take HCL with Gentian Root bitters? While I’m waiting for my Amazon order of supplements to come, I went to see what my local natural food store had – either an HCL with a very low dose compared to what you recommend, or one with Gentian bitters. And for a fairly superficial question: Are you able to have coffee and caffeinated now that your acidity has balanced out, without it provoking reflux issues? I haven’t been able to… Read more »
Hi Jay, No problem. I have not tried HCl in combination with bitters. My tendency would be to just try the HCl as opposed to adding another acid promoter. Not sure how potent the gentian root bitters would be on their on and stimulating sufficient acidity to close your sphincters (which is key to enabling successful transition off of the medications). I personally do not drink coffee. However, I have been able to resume a normal diet since recovering. It has been eleven months or so since I took my last ppi medication and nine months since I recovered. Best… Read more »
Thank you so much for this helpful guide. Trying to get off PPIs for the third time, and having symptoms come back as usual, I was willing to try anything. I was skeptical because it seemed like when I had vinegar in foods (e.g. salad dressings), my reflux would get worse. But I figured why not give it a try at a low dose (2tsp) VERY diluted in water – and to my shock it helped! I just got some ACV pills so that I don’t have to use the liquid, as you recommend, so I can give my esophagus… Read more »
Hi Jay, Sorry for the delayed response. My website server to have had a glitch that held email notifications for the past week. You are very welcome! I’m a huge fan of introducing food diversity, especially fermented foods. In fact, if you read between the lines in my articles the supplements are essentially fast tracking the process of rebuilding a healthy digestive system, complete with probiotic enzymes. I actually wrote a whole section on this in my book that will be releasing shortly. Fermented foods are a great supplement to your recovery. If not for the troubling issue of acid… Read more »
I have severe silent reflux. I also take low dose steroids for an autoimmune disease I have. I see that the HCI shouldn’t be mixed with steroids. Will I be able to get off the ppi meds
and heal my silent reflux with just taking the digestive enzyme and apple cider vinegar pills? Or is there something I could substitute for the HCI that would have the same results since I can’t take it because I’m on the steroid?
Hi Amy, Sorry for the delayed response. My website server to have had a glitch that held email notifications for the past week. You could try substituting digestive bitters for the HCl as I understand they can help to stimulate the production of stomach acid. Just note that I do not have personal experience with these products so I cant vouch for their effectiveness. You know, everyone’s reflux is slightly different. It could be that this combination will be sufficient for you to get off the PPIs and re-build your digestive efficiency. One thing you could try that I have… Read more »
Help Doctors don’t know what I have. They thought I have acid reflux but endoscope found no erosion or cancer and ENt did CT Sinus/facial bones without Contrast and showed no abnormalities I have a metallic taste in my mouth and excess amount of phlegm which drives me crazy. Everything I eat sticks to my teeth. Everthing I drink or eat I have to spit up all this phlegm. (even when I brush my teeth) When I get up in the morning I do the Neti pot and I usually spit up phlegm for an hour or hour and half.… Read more »
Hi Annette, Sorry for the delayed response. My website server to have had a glitch that held email notifications for the past week. Let me say, I am so sorry to hear what you are going through. I pray you find relief soon. If you indeed have acid reflux, the approach on this website may help to address your phlegm issues. It is a common response to the presence of acids / acid vapors in the soft tissues of your nose and throat. I actually just wrote a whole guide on dealing with mucus in my book that I’ll be… Read more »
Hi Don!
I read your article and I was wondering if you recommend these products for singers?
Because I am currently taking silent reflux medication and sometimes it seems like it helps and then the next day, my throat hurts again.
Hi Eliza, Sorry for the delayed response. My website server to have had a glitch that held email notifications for the past week. As a singer, I would be really thoughtful about anything I do that could affect my voice quality (good or bad). For me, it relieved the frequent hoarseness and gurgling that was present in my voice due to the presence of acids on my vocal chord. It was worse after eating. Perhaps you could provide some additional details about your experience such as: how long you have been dealing with reflux, what your diet looks like, what… Read more »
I have had this problem for over 2 years, I eat pretty healthy I would say. No excessive fast food, I’ve tried to stay away from gluten and dairy, but sometimes I’m not successful. I’m not sure what could be contributing to my sore throat, I’ve had my tonsils out and my deviated septum fixed. I’ve taken medication for silent reflux and the normal acid reflux and it didn’t work. I’ve also stopped wearing my retainer, but my voice is still sore, hoarse and other things.
Hi Eliza, It’s hard to say from the information in your question. However, I assume from the way your question is phrased that you suffer with silent reflux which is notoriously resistant to traditional acid reflux medications. If so, the sore throat may be due to the presence of pepsins (digestive enzymes) that have embedded themselves in the soft tissues of your throat. If so you may be able to flush them out by drinking lots of water and avoiding activating them by consuming acidic food and drink. It may not be pepsins though, it could just be the consistent… Read more »
In addition to your suggestions, should I also take the supplements that you’ve talked about and recommend in your article?
Hi Eliza, Yes you are right. If you don’t have it already, you should get my book guide which details the three phase plan: https://theacidrefluxguy.com/book
Best Regards,
Don
Okay! But in addition to the yogurt and other things, should I also try the supplements you have suggested in the article?
I’m so glad I stumbled upon your website. I have literally lost 10 lbs in a week from severe acid reflux. I cannot eat anything! I’m on Mylanta and Tagamet and will meet with gastro virtually this week. When would be a good time to start supplementation? Should I wait to be fully healed or diagnosed officially? I’m miserable right now. After 7 days I finally ate my first meal tonight.
Hi Mariyln, So sorry to hear what you have been going through in recent weeks. If you are meeting with a gastro, you might get some advice from him or her on your plans! Not sure how well versed they will be on alternative remedies, but hopefully they can speak to the underlying root causes of the disease and provide some commentary on the applicability to your situation. I hope you are able to find relief soon :).
Don
Don, I have been through the wringer the past 6 months. I’ve lost 50lbs in a short period of time. I’ve cut out everything – gluten, dairy, spicy, coffee, chocolate, anything acidic – and I have no relief. I’ve had endoscopies, ultrasounds, and saw a naturalist doctor who put me on tons of supplements. I even had my gallbladder removed last week after a gallstone attack! I’ve never had the typical reflux symptoms. Based on my own research, I assume I have LPR but I’ve never had the cough and I don’t really have mucus. It started with a lump… Read more »
Hi Tara, Thank you for your comment. This is such a strange disease and it manifests in so many unique ways. I truly hope you are able to find some relief soon. As you have noted, I wouldnt advise taking ACV in liquid form. It most certainly would make your throat issues worse and overtime lead to other soft tissue or tooth enamel corrosion. Digestive enzymes come in many forms. If you still have that variety you might compare the active ingredients of that brand vs the one I took (essential enzymes). Given your history of digestive challenges, you might… Read more »
I ended up seeing my GI doctor, and I mentioned your regimen. She didn’t believe digestive enzymes were necessary since my pancreatic function labs were OK, and she seemed to have never heard of taking HCl. She never even heard of LPR. I was shocked because she is younger (late 30s?) so I thought she’d be more progressive. She told me to try Pepcid AC, which I did and quickly stopped. She told me to try ACV as well, since she knew of studies that showed it works. I bought the brand you suggested and I felt burning in my… Read more »
Hi Tara, If your sphincters are open you may feel the effects of additional acidity from the ACV as it contains acetic acid. The HCl supplement is primarily geared towards activating your sphincters to close. It’s not surprising that your doctor has never heard of LPR. Most doctors, it seems are not.
Best Regards,
Don
Hi Mr Daniels my name is Caterina and I’m just giving you an update on my acid problem I’ve tried taking the Betaine HCI Chlorhydrate . I took them for about a week but unfortunately I started to experience side effects,they were making me very itchy so I had to stop taking them I’m at my wits end,any more suggestions?
Hi..I don’t even know where to start..been suffering with GERD for more than five years..the medication from the doctor help for a while until I stopped taking them..it’s the worst I’ve felt since I’ve been diagnosed..I read your article and ordered the three bottles of pills..got them yesterday and started taking them..felt a little burning and wondered if it’s normal..I took them twice per day with meals..how long do you think I’ll be seeing results..thanks for sharing your journey..I live in Jamaica so I really enjoy spicy food which I can’t eat now because I really want to get better..I… Read more »
Hi Ann, While you are transitioning away from the reflux medications it might be best to avoid triggering foods (spicy, fatty, etc..). Its not required, but can help you to isolate things that may be triggering your reflux. It is possible that you have not taken enough HCl to affect the closure of your lower esophageal sphincter. If needed, you can check out my book for additional details: https://theacidrefluxguy.com/book
Best Regards,
Don
Hi Don, I have downloaded the guide and I am very excited to try this. I was wondering about the digestive enzymes and ACV, I don’t see any points on when/how often to take these supplements. Should I take one with every meal with the HCI? Or once in the morning? Would love to know how they react with each other. Thank you!
Hi Sarah, Thank you for your comment. I have updated the post to clarify this. I took one digestive enzyme and one apple cider vinegar pill each with meals. The HCl varies by meal complexity: 1 with simple meals, up to 2-3 with most meals, up to 5 with high protein meals like steak or pork chops. I describe this on the article and go into further detail on my experiences in my book: https://theacidrefluxguy.com/book. I cant speak to how they react with each other so much as describe how each work. I provide some additional detail here: https://theacidrefluxguy.com/resources/ Hope… Read more »
Thank you so much for your quick response! It’s very much appreciated.
You’re very welcome!
Hi Don! Thank you for the article! I have sliding hiatal hernia and have symptoms like yours! However, doctors are treating me for high stomach acidity and of course, medications doesnt help! How did you found out you have low stomach acidity? I am feeling i might have it too but doctors say they are sure its high. How to find out its low? Did you also do exercises to treat hiatal hernia? Thanks for the answer! Searching the web for supplements you wrote about!
Hi Anastasija, Thanks for your post. I believe I answered your question via email!
Hello. When I start this regimen do I immediately stop taking my acid reflux pills? I’m scared to stop them and get bad chest pains/burning in my chest from severe reflux. I’ve been taking magnesium and B12 for 2 years now so can I continue to take them while on this regimen? Thank You and pray to god that I am able to finally get rid of my GERD that I’ve had since 03′.
Hi Annette, I took the medications during dinner and was able to skip my medicine the next morning. I have not taken my reflux medications now for 8 months or so! Not everyone has this immediate a response. If that is the case for you, it could be that your does of HCl is not right. If you dont already have my book, you can find it here https://theacidrefluxguy.com/book. Technically, if your acidity is restored you should be able to properly digest and absorb b12 and magnesium. I’m glad you were aware of these deficiencies… I wasnt. The lack of… Read more »
Hi Don! I am so excited to have found this article exclamation since March, I have been having a lot of throat clearing, postnasal drip, etc. and it seems to be in relation to eating. Allergy medications and H2 blockers have not worked. I’m so excited to try this supplement regimen. Did you have asthma-like symptoms? That is the worst for me. You mentioned the ACV, Betaine, and the digestive enzymes, then you said OR are you going to try B vitamins and magnesium. Should it be one or the other, or do you take all five? Which type of… Read more »
Hi Yvonne, I wouldn’t say I had asthma symptoms, more choking, coughing, mucus, and painful airways. Thanks for your question. They ACV, digestive enzymes, and HCl are the main supplements. The b12 and magnesium, I took to help with long term side effects of taking ppi medications. I will actually change that statement as it is a bit confusing, indicating both serve the same purpose. Thanks!
Don
I feel I have had Silent Reflux. Your article has brought to light what I need to do. Thank you so much for sharing!
You’re very welcome. Best of luck with recovery!
I see that you suggest apple cider vinegar supplements but this vinegar makes my phlegm act up so what do I do? I would really appreciate an answer
Hi Caterina, If you are taking Apple cider vinegar in liquid form, this is likely your bodies natural defense to the presence of acid on the soft tissues of your throat. It is also corrosive to teeth enamel so I don’t recommend taking it in liquid for at all, even if diluted or consumed using a straw. Now, if you are taking it in pill form and still seeing this reaction, it is likely because your lower esophageal sphincter is not closed. Apple cider vinegar contains acetic acid, so your body is likely responding in the manner notes above. Lastly,… Read more »
Thank you so much for your reply actually that’s exactly my problem the sphincter doesn’t close so I will buy the supplement you recommended and see what happens thank you again I really appreciate it
I’m curious if you found improvement with the HcL?
Wow, thank you for the thorough and well presented resource on LPR!! Iʻve felt “short of breath” constricted in my throat since March 2020, but the pandemic has made me reticent to talk about these symptoms and unable to get to a doctor. I have had my thyroid tested now and my sinuses scoped, but Iʻm certain the culprit is LPR. It is the worst and the tightness in the throat and airways can get very scary!! I am really stoked to try your recommendations. Since I am just now figuring out that this is LPR, I have a prescription… Read more »
Hi Beth, Thank you for your comment. With regards to how quickly you feel better, everyone’s different and it has a lot to do with getting the right dose of HCl. If you dont already have it, I provide additional details in my book: https://theacidrefluxguy.com/book. I didn’t request a blood test to verify my B12 deficiency. After reading the side effects there was absolutely no question in my mind that I had it :). Nearly immediately, my sleep improved, the sensitivity in my fingerprints went away, my sense of touch became more acute, my brain fog dissipated, my concentration approved,… Read more »
Hi Don, I am not completely sure if I have just the condition, Post Nasal Drip or Silent Reflux, I have had colds on and off for the past 6 months. I have been to the doctors a number of times, he thought it maybe acid reflux. He gave me a prescription for Somac, I didn’t really stay on it long because I wanted to find out what my problem is. I have never been the type of person to take any medication, I always prefer a natural way to go. My doctor in the end said its a bit… Read more »
Hi Cherie, I am sorry for the late reply. For some reason, I didn’t see a notification of your comments. As you have indicated, it can be hard to tell if your post nasal drip is bacterial, viral, or due to silent reflux. However, if you understand the reasons for reflux induced post nasal drip, you can more easily diagnose. The reasons you get post nasal drip from reflux, is your body will naturally release a protective coating of mucus to minimize damage in the presence of acid vapors. That said, if you determine your nose starts running backward into… Read more »
Hi Don, I feel like I needed to find this article so bad! I’ve been suffering from the feeling of lump in my throat feeling like I can’t swallow, hoarseness, inflamed larynx, burping, anxiety, chest tightness feeling like I can’t get a deep breath. EVERYTHING! I’ve been to all the “ologists” . I got the flu back in December then started having all of these symptoms. I got tons of bloodwork where they said I have an under active thyroid and was told I had to start medication for that. I was having dizzy spells heart palpitations, and started having… Read more »
Hi Paige, Yes the supplements are temporary! They enabled me to get off of the reflux medications immediately and after 8 weeks I got off of the supplements as well. Sounds as though your reflux was triggered by the flu or medications, which can happen. Hope you are back to normal soon!
Don
You sound like me! I have almost the exact same symptoms
Hi Don, Doctor diagnosed me with GERD last March. It went off for a good three months until end of June. This time, I didn’t have bloating or excessive burping but more of the throat symptoms such as a lump sensation on the throat, and sometimes it feels like there’s something poking my throat and I will occasionally get upper back pain too. I’m suspecting that this could be LPR? I just went to the doctor last weekend and he prescribed a 2weeks dose of PPI (rabeprazole). In 3 days of taking the medicines, I am not really seeing any… Read more »
Hi Roselle, The globus (feeling of a lump in your throat) and back or chest pain are common symptoms of LPR so it could be. Also, LPR is notoriously resistant to acid reflux medications. One of the tell tale signs is excessive mucus or nasal drainage. If you find the right dose of the supplements you should not need to take your medications. I have heard of people taking them at the same time and slowly weaning off of medications. As you might expect, that is a very slow process as the two counteract each other. The supplements encourage restoration… Read more »
How long did it take you to heal using the supplements? Thank you for all of this information. It has been awful and I am looking to heal. It has been a long journey and I was on PPI’s for three months and had terrible side effects. I have been off of them for almost two months.
Hi Maria, Thank you for your comments. I am happy to hear you have weaned yourself off of these terrible medications. My symptoms got so bad that I couldn’t go without them or handfuls of antacids for more than a couple hours! That said, the supplements enabled me to get off the medications without devolving into a coughing hacking mess! In fact, most of my symptoms were eliminated fairly quickly (so long as I took the supplements and in the right quantity) For me, it took 8 weeks to get back to normal. After that, I was able to get… Read more »
Maria, Thanks again for your question! It will hopefully help countless others as I have added this response to the top FAQ: How long did it take you to heal using the supplements?
Thank you so much Don. I am hopeful that I can heal from this. The silent reflux is terrifying. Just grateful there are wonderful people out there like you trying to help others heal.
Hi Don! So happy I found you, hope I can heal myself with these tips. I was diagnosed, simply, as having acid reflux by my GO and we did a couple of rounds of Prilosec and another. My naturopath, however, advised against it and told me to take DGL instead. Helped for periodic episodes. I have allergies and have had post nasal drip for some time, not sure if it is due to allergies or reflux. Over the past year I have woken with some pretty severe sore throats, thought I might have snored during the night. I did figure… Read more »
Kathleen, So glad you found the site! Just one thing to consider is taking ACV in pill form vs liquid. The reason is it contains acetic acid and is corrosive to teeth and soft tissues (throat). This is still the case if you dilute it or drink it with a straw. Would hate for you to improve your reflux situation only to find that you have irreparably damaged to your teeth or throat. I have not shared any details yet about the book. I am actually taking a little break from writing to respond to your comments :). Recognizing this… Read more »
LPR- hello Don, how are you? I hope you are well, I messaged in your Instagram account. I believe I may have LPR and have had acid reflux in the past. I’ve beeb going through it for the last 3 months. I’m lost on what to do and don’t want to take PPIs. I’ve got wheeziness, hoarsness – agony when I talk, throat pain that’s constantly there, coughing clearing throat, stomach/body pain as if I can feel the acid literally burnt I feel my body I wake up in the night or in agony, it goes to my right ear… Read more »
Hi Anj, I have also responded to your direct message on IG, so feel free to respond via either channel. First, I am sorry that you are facing this. I suffered with GERD for more than 15 years and LPR for the six months preceding my recovery. That said, I did not experience it to the level you describe. Per my personal experiences and the research I have done, I am convinced that most people experience reflux because their bodies are unable to properly close the junction between the stomach and the throat. This is particularly important for those with… Read more »
Have your symptoms gotten better? I am in the exact situation as you and it is horrible. I am in the process of seeing a therapist to deal with my anxiety, while dealing with acid reflux. It really is a stressful situation, but I am optimistic that I can get better!
I’m hoping Don Daniels gets back to me with his guide. I really want to try this the natural way and avoid the medication because I do not want to depend on it for the rest of my life.
Hi Victor, Yes I have been reflux free now for about 6 months! I stopped taking my reflux medications once I started the supplements and 8 weeks later no longer needed the supplements. I have been off all medications and pills since that time. Wish you best of luck is you decide to try this approach!
Don
That’s great to hear!!!! I’m currently on medication, and I have not bought the supplements yet. How would I transition from not taking the medication to taking the supplements? Also, is it possible for you to send me your guide? I know you said it is important to take the right dosage of HCI, I want to make sure I do it correctly.
Hi Victor, You can get my book here https://theacidrefluxguy.com/book
Thank you so much! I’m about to purchase all three supplements. Nothing but good reviews, so I’m confident in myself and in the supplements that they will help me. So glad I found you!!! I just started the medications about 7 weeks ago, and like you doctors told me to take this for 6-8 weeks. I’m close to being done with the medication, however, they just told me to continue to take them for an additional 6-8 weeks, and although they have helped a bit (not entirely) I know that I do not want to to continue taking these medications… Read more »
I am so grateful to have found you. You have no idea. I have been suffering severely with acid reflux/GERD for over 12 years and all the symptoms you explained in the article happened to me slowly but surely. I never stopped to address it, so recently within the last six weeks I had a horrible experience and I am healing from it now. Because of the pandemic all the doctors wanted to do was test me and give me allergy medicine and none of it worked! I got doctor bills for no reason. Not one of them diagnosed it… Read more »
You’re very welcome! Let us know how it goes 🙂
Hi Don…thank you for so much insightful information. I have all of the symptoms of awful digestion and reflux. It is making my life completely miserable cause I really cannot eat much. The dr has me on a strong ppi which I realize I need to get off. I really don’t believe it is helping much at all. I am taking a digestive enzyme but the idea of taking an acv supplement and the hcl terrifies me. The worst symptom is shortness of breath and all of the typical lpr symptoms. If I were to take these supplements, would it… Read more »
Hi Gina, Thank you for your comment! So sorry to hear about your experiences. Are you unable to eat due to throat swelling or inflammation? One key difference to note with the ACV supplements is they do not activate until they are in your stomach. It sounds as though you were taking the liquid form and even in the best case (when diluted with water) it can have corrosive effects on your throat and teeth as they go down, especially if they are already inflamed. Regarding the HCL and ACV, I can only share my experience as there is limited… Read more »
Hello, I think/believe silent reflux and it sucks. All the medication I’ve been taking hasn’t helped. I’m constantly burbling, I feel like I have something stuck in my throat and starting to experience anxiety cuz of all of it. I truly need your help to get better.
Hi Rosio, Silent reflux certainly sucks! One way to distinguish silent reflux from traditional reflux / GERD is if you experience post nasal drip or mucous in your nose, throat or mouth. This occurs as your body’s natural response to the presence of acid vapors. Regarding your throat, it sounds as though you are experiencing globus, which can often be a swelling of the tissues surrounding your lower esophageal sphincter. The burbling may be your bodies attempt to distribute low stomach acid to properly digest your food. Do you have any specific questions that I can help with?
What foods are you able to eat now ?
Hi Jess, Thanks for the question. I eat everything now! Of course, while I was healing, I took care with what I ate so I could clearly distinguish reflux triggers.
How is your acid reflux to this very day?
Hi Stephon, My reflux is thankfully non-existent! You remind me, that I have been intending to add my experiences with the supplements. Specifically how to determine proper doses and how to adjust as that changed throughout my recovery. Ultimately your body signals you at each step until you are completely off of the supplements.
Don had a question regarding the source natural essential enzymes, hcl betain both which I started 3 days ago, in the morning I tend to have a muffin, banana, and chamomile tea, I am noticing the past 2 days that I get stomach cramps/hot feeling with them in the morning. Could this be that I am taking to small of a breakfast for the enzymes, should i stop? Additionally, for 2 bigger meals the betaine hcl made me feel better on 2 pills, yesterday during lunch the 1 enzyme pill and 2 bcl pills caused me some bloating for most… Read more »
Hi Anthony, Thank you for your question. Glad to hear you have seen some relief as you are finding the right dose of the supplements. Means you are on track! Yes, HCl doses should correspond to the digestive complexity and size of your meal (does not mean it is only used with protein). You have noticed that you get a warmth feeling when you take it with easier to digest meals such as you have mentioned with your breakfast. A few things 1) After a few days, you have noticed a change in your bodies response to the HCl. This… Read more »